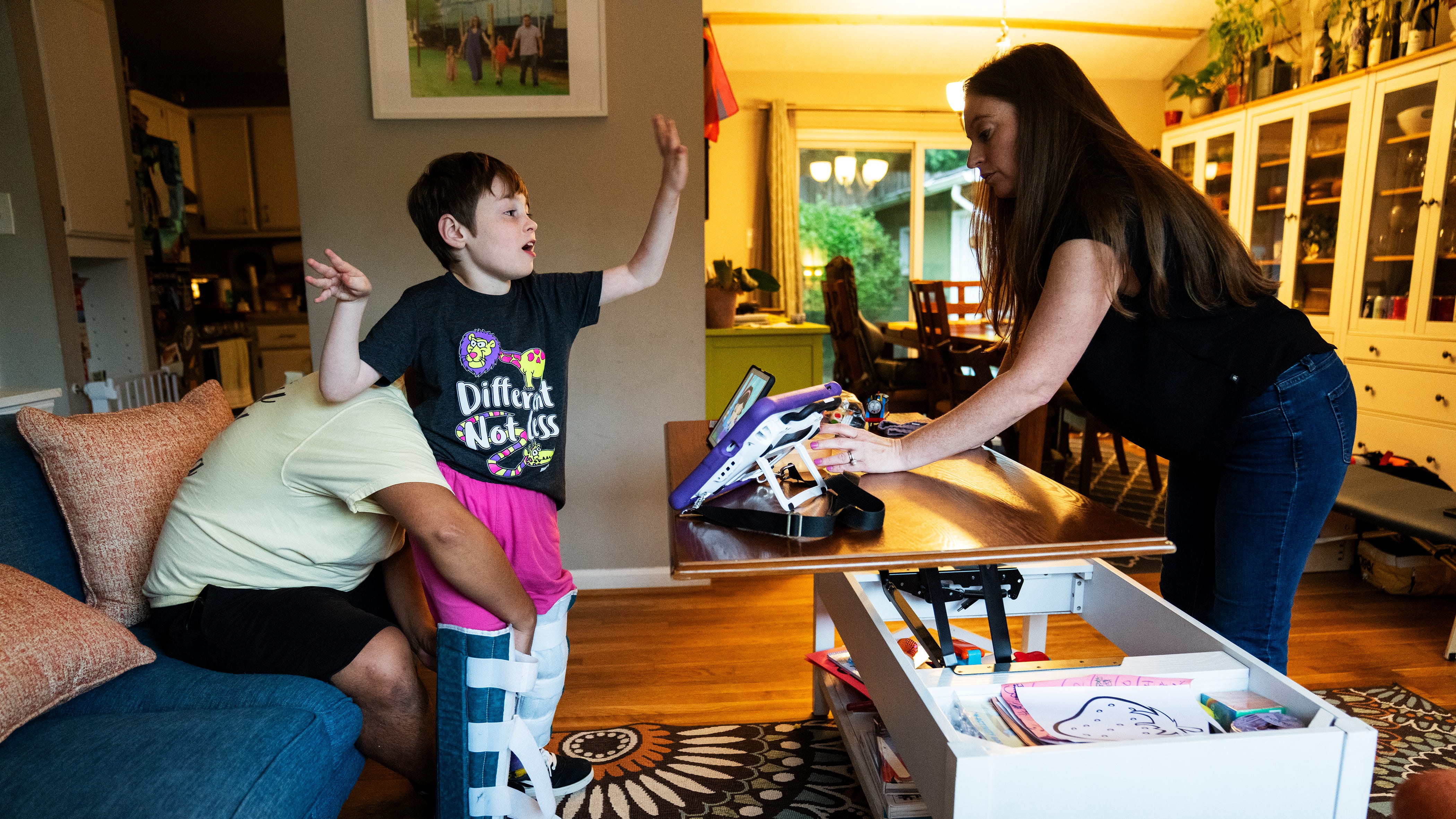
How future Medicaid cuts could negatively impact children with disabilities
Parents of children with disabilities argue that Medicaid cuts in the One Big Beautiful Bill will directly impact their children’s well-being.
Shumeeka Simpson, an Omaha resident, works as a patient navigator for the American Civil Liberties Union, an administrative assistant for Nebraskans for Peace, and shifts at a Dunkin store.
Still, even those with three jobs worry they will lose their health insurance when Nebraska becomes the first state on May 1 to require certain Medicaid enrollees to work, train and attend school under rules mandated by Congressional Republicans’ One Big Beautiful Bill Act.
Simpson, 46, has relied on Medicaid since her divorce in 2014. None of her employers offer health insurance. She said technical issues prevented her from updating in time, causing her to lose federal food aid, and she doesn’t trust the state to implement the new work rules without a hitch.
“Adding more barriers doesn’t make the program work better,” she says.
Nebraska Medicaid officials said they are working to make compliance as easy as possible for enrollees so that people don’t lose coverage for administrative reasons such as failing to submit proper documentation.
Enrollees with any of the thousands of health conditions detailed by the state will be exempt.
“Our top priority is to provide members with a clear understanding of the changes to the program and how to maintain coverage,” Drew Gonshorowski, the state’s Medicaid director, said in a news release in early April.
Centers for Medicare and Medicaid Services Administrator Mehmet Oz said in a brief interview with KFF Health News on April 28 outside the National Press Club in Washington, D.C., that he applauds Nebraska for being the first state to begin implementing work requirements. He acknowledged that the state is still “working through the issues,” adding that he hopes “by the end of this year, we’ll be in a more sophisticated situation.”
But health policy analysts, advocates for the poor and health care industry groups remain skeptical, fearing that thousands of Nebraskans on Medicaid will lose coverage and, with it, access to medical services and protection from medical debt.
Jeremy Nordquist, president and CEO of the Nebraska Hospital Association, said hospitals are also concerned that an increase in uninsured patients will hurt their bottom line.
“There’s a lot of concern at different levels,” he said. Many enrollees may not be aware of the change and may not realize they must take action to continue their coverage, he said.
The law signed by President Donald Trump last July requires the 42 states and the District of Columbia that fully or partially expanded Medicaid under the 2010 Affordable Care Act to implement work requirements starting in 2027. The full expansion would allow adults with incomes up to 138% of the federal poverty level, equivalent to $22,025 for a single person this year, to qualify for Medicaid, a government program for low-income people. income or disability.
More than 20 million people gained Medicaid coverage through the expansion, according to KFF, a health information nonprofit that includes KFF Health News. The Congressional Budget Office estimates that 4.8 million people will become uninsured over the next 10 years due to work requirements.
Under the law, enrollees must work or volunteer at least 80 hours a month, attend school at least part time or participate in job training. Or you must prove that you qualify for certain exemptions, such as caring for a child under 13, a disabled parent, or having a medical condition that prevents employment.
Some states were considering implementing labor regulations several years before the law was passed. This gave states the option to start the program early.
nebraska state plan
About 70,000 Medicaid enrollees must meet the requirement, which Nebraska implemented eight months before the law requires, said Colin Spirinek, a spokesman for the Nebraska Department of Health and Human Services.
About 72% of them probably won’t need to do anything to stay insured, Spirinek said. That’s because states already track their employment and exemption status through state or national databases.
To check whether enrollees meet the requirements, Nebraska and other states plan to tap a variety of databases, including Medicaid claims information and data maintained by credit rating agencies. Registrants without data in Nebraska will receive a notification and can complete an online form to confirm they meet the new rules.
While many states have said they plan to hire additional administrative staff, the Nebraska Medicaid Agency has not added employees to meet operational requirements.
“The fact that they’re saying they don’t need additional resources begs the question of whether they can get this done without future headaches,” Nordquist said.
Although documentation is required to prove employment status, Nebraska officials will allow enrollees to self-certify that they volunteer, attend school or qualify for an exemption, such as caring for a parent with poor health or a disability. “Supporting documentation such as medical records is not required,” Spirinek said.
This could make registrants more likely to receive exemptions under the law’s “medical frailty” exception. A long list of medical conditions eligible for exemption was released by the state last week, including many types of cancer, mental health, heart disease and more.
Kelsey Allens, senior staff attorney at the advocacy group Nebraska Appleseed, said the state’s long list of medical billing codes for exempt conditions is still insufficient. He said different levels of disease severity were not included.
The waiver is critical for Crystal Schroer, 30, who will receive Medicaid starting in 2022 and be unemployed since 2024. She said it was difficult to find a job near her home in Kearny, Nebraska, that would allow her to take Tarot, a psychiatric service dog who helps with anxiety, with her.
“I’m really worried,” said Schroer, who lives with a friend. “It made my depression even worse.”
Whether self-certification will be widely accepted in other states will depend on CMS work requirements rules expected to be enacted this summer. “We don’t like self-certification,” Oz told KFF Health News. “Documentation is important.”
Several advocacy groups, including the American Diabetes Association, the HIV+Hepatitis Policy Institute, and the National Bleeding Disorders Foundation, had asked states to exempt registrants under certain conditions. The group said losing insurance coverage means losing access to medicines that keep people healthy and avoid hospital visits.
Adding work requirements to Medicaid has been a priority of Trump since his first term. In 2018, his administration allowed states to adopt the policy for the first time, but only Arkansas did so. More than 18,000 people lost their insurance in the nine months after the policy was introduced until a federal judge ruled it illegal. This equates to almost one in four people covered by the obligation.
In most cases, you lose coverage not because you didn’t meet the requirements, but because you didn’t submit your documents correctly by the deadline.
In Georgia, work will be required starting in 2023 under a partial expansion of Medicaid. Only about 8,000 people signed up for coverage in the first two years, far fewer than the 25,000 that state officials expected in the first year alone, and many were denied benefits due to red tape.
national mission
During Congressional debate over the law last year, Republicans pushed Medicaid work requirements as a way to recruit “able-bodied” adults into the workforce who would benefit from government assistance. House Speaker Mike Johnson said it will help keep Medicaid “for the people who deserve it,” not young people “sitting on the couch playing video games.”
Republicans argue that the employment mandate would encourage people to find work and leave Medicaid to help children and people who are pregnant or disabled.
They were unfazed by the study’s finding that most adults receiving Medicaid are already working, attending school, or have health conditions that prevent them from doing so.
A recent study published in the Annals of Internal Medicine found that about one-third of adults at risk of losing insurance coverage under new work requirements report having a physical or mental illness or disability.
“This doesn’t mean that most healthy adults are choosing not to work,” said study co-author Darshari Vyas, a health policy researcher at Beth Israel Deaconess Medical Center in Boston. “This is a vulnerable group and we don’t know if there will be clear protections when we start introducing work requirements.”
In Nebraska, about two-thirds of Medicaid expansion enrollees are working or attending school, according to KFF. Nebraska’s unemployment rate is 3%, one of the lowest in the nation.
Andrea Skolkin, CEO of Omaha-based One World Community Health Center, said this is an anxious time for the clinic and its patients. “We remain concerned that people eligible for expanded Medicaid will lose coverage,” she said.
About 4,000 of the 52,000 patients are eligible for Medicaid expansion, Skolkin said. He said many admitted students have received letters from the state regarding work requirements, but he is concerned that many do not understand them.
Losing 10% of those patients would mean a $500,000 decrease in revenue for the nonprofit center, she said. To assist patients, the company plans to hire more staff to help fill out forms to obtain and maintain insurance.
Allens, of Appleseed, Nebraska, said he is skeptical of the state’s promise to use automation to ensure enrollees meet work requirements. “We remain very concerned about early implementation,” she said.
The federal law also reduces retroactive eligibility for expansion enrollees from three months to one month, which could make it harder for people who lose insurance to get coverage for their medical bills when they re-enroll in the Medicaid program.
Nordquist said hospitals are concerned that the change could leave health care providers paying more if they lose health coverage, since many people enroll in Medicaid when seeking emergency care, and enrollment can take weeks or months to complete.
Only two other states have plans to implement this work requirement early. Montana is scheduled to start in July and Iowa is scheduled to start in December.
Andrea Maresca, senior principal at consulting firm Health Management Associates, said many states will be watching Nebraska’s implementation closely to see what lessons can be learned before implementing their own in January.
States are better prepared to enact work requirements than they were when Arkansas went to court in 2018, she said. After re-verifying the eligibility of millions of registrants post-COVID-19, they have more experience using public and private databases to automate processes and have more practice communicating with registrants, Maresca said.
Still, “it’s not perfect,” and states will have to adapt accordingly, he said.
KFF Health News is a national newsroom that produces in-depth journalism on health issues and is one of our core operating programs. KFF — An independent source for health policy research, polling, and journalism.
(This story has been updated to add new information)

