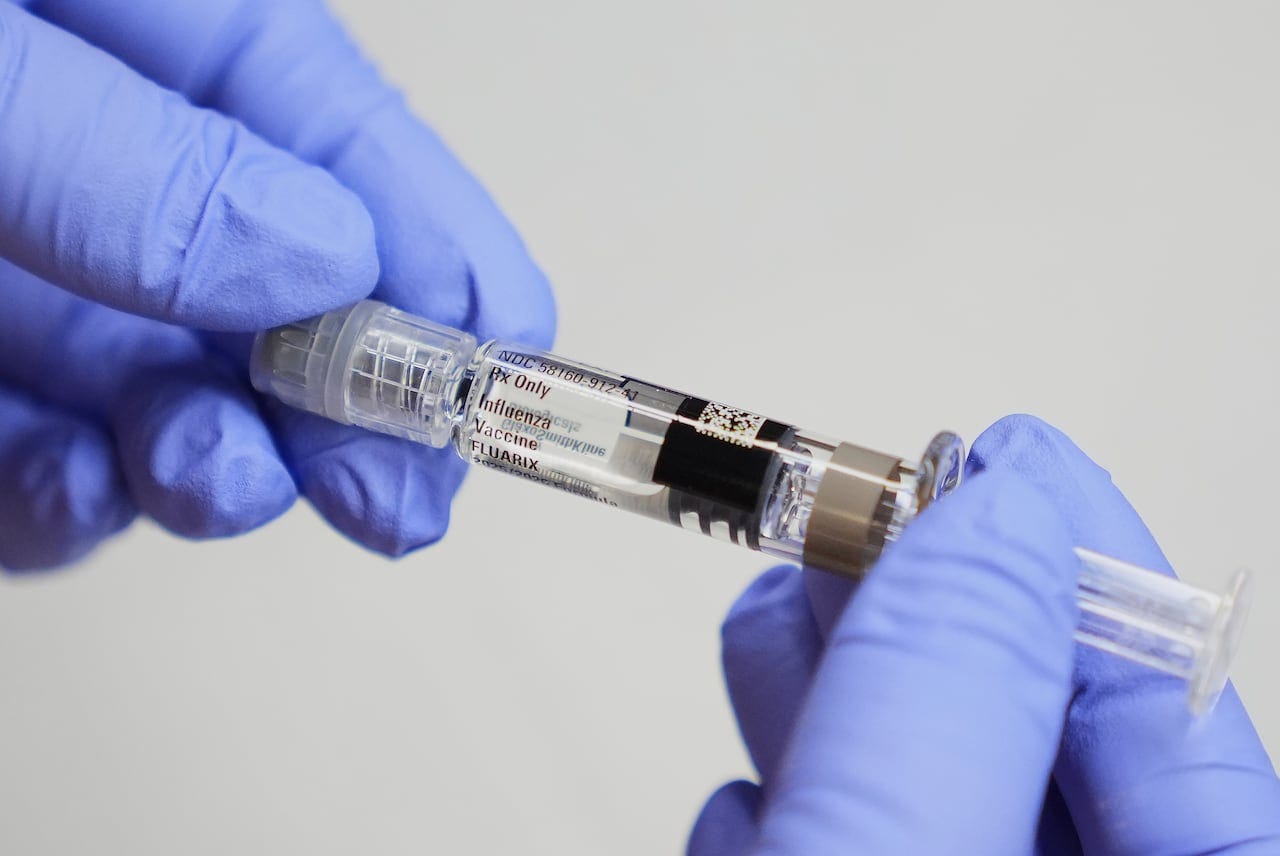
Should you get a flu shot? Experts say yes
Mutations in some H3N2 strains may not match current flu vaccines, but doctors explain why it’s still a good idea to get vaccinated.
CBC – Top Stories
It’s normal to feel tired after a busy week, a bad night’s sleep, or a lingering cold. However, for some people, the feeling of fatigue persists even with rest. It will be a constant and helpful companion with which you can rebuild your daily life.
These people may have trouble concentrating at work, keeping up with social commitments, and may even find it difficult to perform basic tasks without feeling drained. For them, fatigue is more than just fatigue. This is a severe system-wide shutdown that does not respond to coffee, naps, or willpower.
This often misunderstood condition, known as chronic fatigue syndrome, is a complex disease that researchers are only beginning to fully understand.
Here we explain what it is, why it occurs, and how people diagnosed with it can find relief.
What is chronic fatigue syndrome?
Chronic fatigue syndrome (CFS), also known as myalgic encephalomyelitis (ME), is a long-term, multisystem disease characterized by deep, persistent fatigue that does not improve with rest and is severe enough to interfere with daily life. “The core of this disease manifests as severe, disabling fatigue that lasts for six months or more,” says Dr. Hector Bonilla, a clinical professor of medicine and infectious disease expert at Stanford Health Care.
According to the Centers for Disease Control and Prevention, as many as 3.3 million people in the United States suffer from the condition, but many go undiagnosed because CFS is often misunderstood or confused with other health problems.
Another difficulty in diagnosis is that the symptoms of CFS overlap with conditions such as depression, hypothyroidism, fibromyalgia, anemia, autoimmune diseases, and sleep apnea. Often these other causes must also be ruled out. Additionally, there are no blood tests or biomarker tests for CFS, so clinicians must rely on a patient’s detailed medical history, symptom patterns and pre-established clinical criteria, Bonilla said.
A characteristic symptom of CFS is “post-exercise malaise,” a delayed decline in energy and function that occurs after minimal physical or mental activity, Bonilla notes. People describe this crash as feeling flu-like, heaviness, cognitive fog, or completely depleted, and it often takes several days or more to recover. Other common symptoms of CFS include “dizziness, muscle and joint pain, lack of sleep, and memory problems,” says Dr. Neha Vyas, a family medicine physician at the Cleveland Clinic. “Sometimes we also see exercise intolerance and decreased peak oxygen consumption.”
Many patients also experience autonomic nervous system problems, such as increased heart rate when standing.
What causes chronic fatigue syndrome?
Although the exact cause of CFS remains unknown, research increasingly points to a combination of biological triggers and chronic dysregulation in multiple body systems. “More than 60% of patients mention a previous infectious process that triggered their illness,” Bonilla says. Such infections commonly include the Epstein-Barr virus, influenza, or more recently, coronavirus disease (COVID-19). “Herpesviruses, enteroviruses and retroviruses are also thought to be involved in this condition,” Professor Vyas added.
These viruses and infections can cause CFS by disrupting immune signaling, energy metabolism, and autonomic nervous system function, and persisting long after the initial illness has subsided, Bonilla said.
Genetic predisposition may also play a role, Vyas said, as studies have shown that people with a family history of autoimmune or immune-related diseases may be at higher risk of developing CFS. Hormone imbalances, particularly those related to cortisol control, have also been observed, but researchers have not yet determined whether these are the cause or effect of the symptoms.
Some people also develop CFS after physical trauma, significant stress, or environmental exposure, suggesting there may be other routes by which the condition develops.
How is CFS treated?
There is currently no cure for CFS, but effective management can significantly improve quality of life. Because symptoms can vary widely, “treatment focuses on managing symptoms, improving sleep quality, addressing pain and cognitive symptoms, and finding ways to improve daily functioning,” Vyas says.
Medical treatment may include medications to manage pain, sleep disturbances, dizziness, and depression, as well as treatment for related conditions such as POTS and allergies. Specifically, some patients may benefit from low-dose naltrexone, antihistamines, or targeted antivirals and immunomodulatory treatments, but the evidence is mixed and expert supervision is required.
Cognitive support strategies such as memory aids and occupational therapy can also be helpful in daily life. Bonilla points out that nutritional guidance is also common, such as eating more whole foods, lean proteins, and anti-inflammatory fruits and vegetables while cutting back on processed foods and added sugars, which can worsen inflammation and cause low energy.
One of the most important interventions at home is pacing, Bonilla explains. This approach involves carefully tracking your energy levels, recognizing early signs of overexertion, and balancing rest and activity to avoid causing a crash. Gentle stretching, hydration, and a sleep-stabilizing routine may also reduce symptoms, but strenuous exercise can worsen post-exercise fatigue and is usually not recommended.
Many patients also find relief from symptoms through mindfulness practices, breathing techniques, relaxation techniques, or support groups that provide emotional and practical guidance.
Bonilla said doctors can adjust recommendations for a particular patient, rule out other illnesses and adjust testing and treatment needs.
Vyas said that while CFS is “a complex and difficult disease that we are still learning,” many people diagnosed with CFS learn how to manage their symptoms more effectively over time. And with new research and growing awareness, there is real hope that better treatments and clearer answers are on the horizon.

