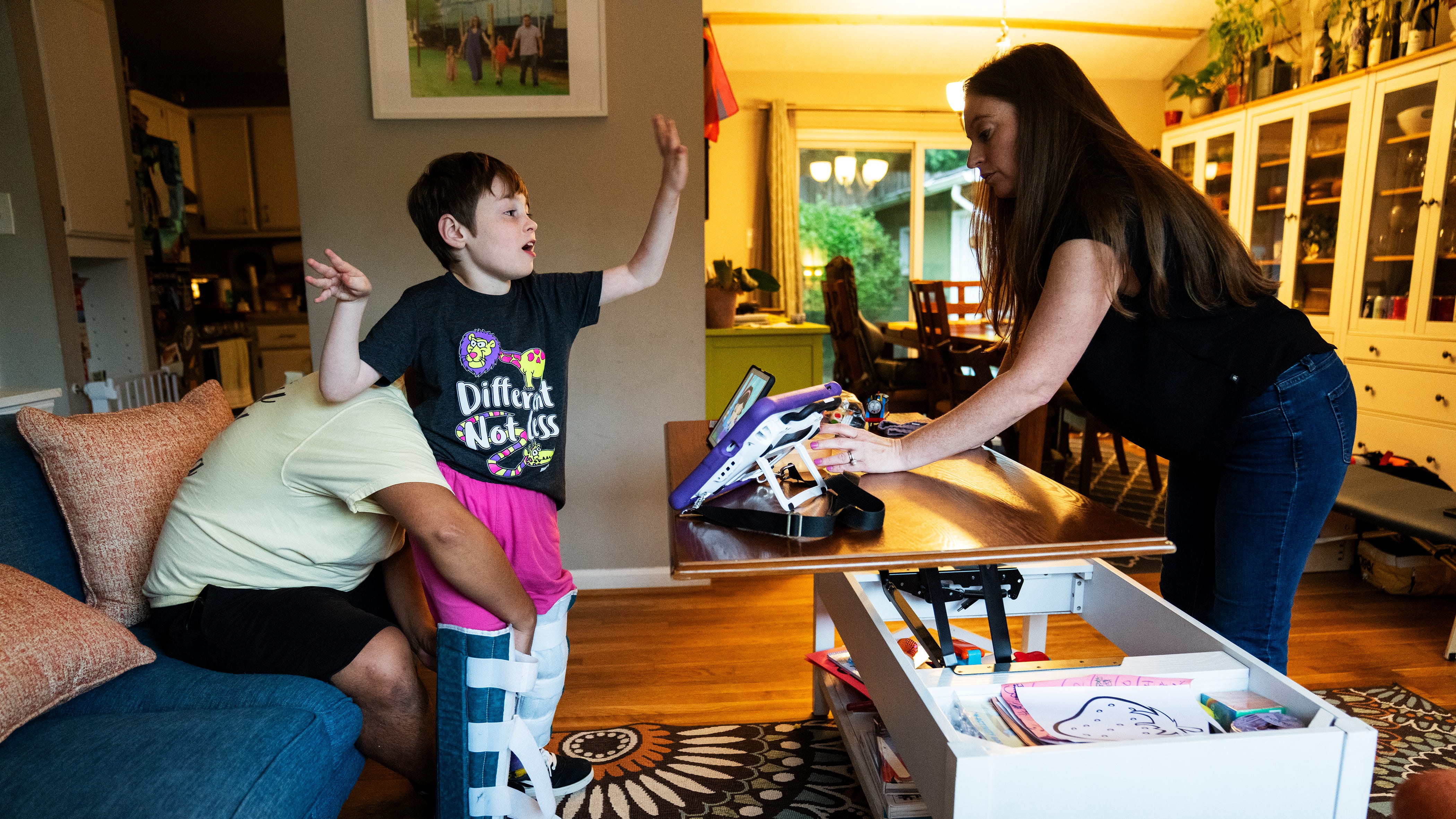
Future Medicaid reductions could hurt children with disabilities
Parents of children with disabilities say that Medicaid reductions in “One Big Beautiful Bill” directly affect their child’s well-being.
If you sign up for MaineCare or Medi-Cal, you may have a decent idea as to which states will offer health insurance coverage.
But what happens if you sign up for a plan under a healthy connection? That’s what South Carolina calls the Medicaid program.
Medicaid is a federal national health insurance program for low-income families that provides health insurance to more than one in five Americans. President Donald Trump’s Tax Cuts and Expense Act will cut more than $900 billion in federal spending on Medicaid over the next decade. According to estimates from the Non-Participation Congressional Budget Office, the law leaves 10 million Americans uninsured over the next decade.
Despite extensive media coverage of the law Trump called the “big beautiful bill,” health advocates say millions of consumers who could be affected by Medicaid and the cuts in affordable care laws will not necessarily be gradualized over several years.
In fact, experts said many people may not be aware that they are using Medicaid.
“Sometimes, people who use Medicaid don’t even realize it’s Medicaid because it has different names in different states,” said Arica Sanchez, health care director at the New Mexico Center for Law and Poverty.
New Mexico’s Medicaid program guarantees 34% of the state’s population, according to a February 2025 report by the Health Policy Non-Profit KFF.
New Mexico tapped four private insurers to manage Medicaid coverage under what the state calls turquoise care. According to KFF, this is one of 42 states that manage one or more categories of private companies called managed care – known as managed care – Medicaid coverage.
Sanchez said consumers could be confused because “when they look at New Mexico insurance cards, they’d say it’s turquoise care that isn’t necessarily Medicaid.”
A more complicated problem is that consumers often get Medicaid coverage despite private insurers controlling their profits. Consumers may think that if they are enrolled in a Medicaid plan managed by well-known insurance companies such as Blue Cross Blue Shield or United Healthcare, they have private insurance companies.
Four Medicaid plans for Turquoise Care include Blue Cross Blue Shield in New Mexico, Molina Healthcare in New Mexico, Elders Health Plan, and United Healthcare Community Plan in New Mexico.
Some states have rebranded the program to prevent the name Medicaid from appearing on insurance cards or communications.
Arizona calls the program the Arizona Healthcare Cost Containment System, or AHCCCS, pronounced “access.” The California Medicaid program is Medi-Cal.
Decision makers often try to identify unique names for their states, according to Jennifer Tolbert, the associate director of the Medicaid program and KFF uninsured.
Some states turn to university mascots and nicknames when branding Medicaid programs. The Oklahoma program is paying attention faster. Wisconsin offers Badger Care. Washington state is dubbing the Medicaid program Apple Health.
Stigma, politics motivates Medicaid rebranding
Many states are renaming their Medicaid plans to avoid stigma that may be associated with government-provided health programs. Joshua McClain, a professor of political science at the University of Utah who co-authored the study, said that ensuring that it is covered by coverage doesn’t seem to be much different from what consumers pass an employer-provided insurance plan.
In 2024, for example, Humana, a researcher at the University of Utah Harvard University and insurance company, looked into the perceptions of more than 5,800 consumers who were asked about the name of Medicaid. When the program replaced Medicaid with a nationally specific name, it was likely that consumers would conclude that they had not heard enough to say how they felt about the program.
In the study, rebranding Medicaid under state-specific program names “disrupts understanding of the program as a government-provided benefit.”
McCrain said some states are likely to rebrand their Medicaid plans for political purposes too.
Former President Barack Obama’s 2010 Health Care Act Affordable Care Act gave the state the option to expand Medicaid for low-income adults. All but 10 Medicaid is expanding, but some Republican-led states have done so on their own terms.
Under former Republican government in Indiana, Mike Pence, called the Medicaid expansion, it required subscribers to pay monthly premiums to manage their health savings accounts. The former vice president during Trump’s first term said he stressed his personal responsibility.
Following Indiana, it submitted a waiver to the Centers for Medicare and Medicaid Services, which seeks to implement work requirements for low-income, non-disabled adults seeking Medicare coverage. The Biden administration blocked such exemptions during the Covid-19 pandemic. However, the work or volunteer duties against Medicaid compensation are pillars of Trump’s tax cuts and spending law.
Now the only state with Medicaid work requirements, Georgia is giving low-income adults a Medicaid opportunity based on their path to coverage programs. The program extends coverage to low-income, non-disabled adults who work at least 80 hours or who are eligible for exemptions such as full-time students and volunteers.
However, McCrain said it is unclear whether changing the name of Medicaid would make a difference in public perception.
When people learn that Medicaid provides medical access to low-income Americans, they generally support the program, he said. However, some political leaders, especially Republicans in conservative states, may find it useful to rebrand Medicaid when they are trying to pass the law.
“It could be, (the name change) had to be done in that political moment to get it through,” McCrain said.

